Article Text
Abstract
Background Bowel obstruction is a common surgical emergency in newborns. One-fourth of neonates with obstruction suffer postoperative complications, with high mortality, especially in low-income countries. Factors attributed to mortality include prematurity, late presentation and associated multiple congenital anomalies. The prevalence and the predictors of mortality in our setting have not been well studied. We aimed to describe the early postoperative outcomes and to determine the predictors of mortality among neonates with bowel obstruction.
Methods We conducted a prospective cohort study during 4 months, when we recruited postoperative neonates from the pediatric surgery unit of Mulago Hospital. We collected data on demographics, clinical presentations, maternal characteristics, the surgical procedure performed, postoperative outcomes, etc. After follow-up for 2 weeks, we analyzed the data using Cox proportional hazards regression models of predictors of mortality.
Results A total of 76 neonates were recruited, with a male-to-female ratio of 2.2:1. The age ranged from 1 to 26 days, a median of 3 [interquartile range (IQR): 2, 7]. About 67.1% had birth weights ranging between 2.5 kg and 3.5 kg, a mean of 2.8 [standard deviation(SD)=0.64]; 76.3% were termed; with anorectal malformation (ARM), 31.6% as the leading cause, followed by jejunoileal atresia (JIA), 25%. Nearly 55.3% of neonates developed complications; 53.9% with post-operative fever, 15.8% had wound sepsis. The mortality rate was 44.7% (34/76) and was highest among cases of JIA, 41.2%. The predictors of mortality included prematurity, fever at admission, breastfeeding status, and mother’s parity as well as the cadre of healthcare providers (p<0.005).
Conclusions ARM is the predominant cause of bowel obstruction among neonates, followed by JIA. The morbidity and mortality due to bowel obstruction among neonates are unacceptably high. The major predictors of mortality were prematurity, fever at admission, and the cadre of the healthcare providers.
- neonatology
- child health
- congenital abnormalities
- gastroenterology
- hospitals, pediatric
Data availability statement
Data are available upon reasonable request. The data used to support the findings of this study are available from the corresponding author upon request.
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.
Statistics from Altmetric.com
Key messages
What is already known on this topic
Bowel obstruction is a common health problem among neonates worldwide.
The pathological sequelae are poorly tolerated by most neonates.
Predictors of mortality are late presentation, prematurity, and congenital anomalies.
The mortality rate is still high especially in the low-income and middle-income countries.
What this study adds
The duration of surgery, as well as the presence of congenital anomalies in association with bowel obstruction, did not affect the outcome.
Neonates who presented early to the health facility had a higher rate of mortality.
Similarly, being a first-time mother was associated with increased mortality rate.
How this study might affect research, practice or policy
First and foremost, the identification of predictors of mortality formed a basis for prevention and prompt interventions in neonates with bowel obstruction.
Second, the findings provided evidence to support resource allocation toward neonatal surgery.
With this background, we foresee a reduction in the mortality among neonates with bowel obstruction in the near future.
Introduction
Globally, bowel obstruction among neonates occurs in 1 of 2000 live births and is responsible for about 28.3% of neonatal admissions.1 2 The common causes include intestinal atresia, Hirschsprung’s disease (HD), and anorectal malformation (ARM).3–5 The cardinal features are bile-stained vomiting, failure to pass meconium, and abdominal distension.3 6 7 Though none of these features are pathognomic, all are consistent with an obstructive phenomenon.8 Jejunal atresia is usually associated with maternal polyhydramnios, which requires prenatal ultrasound examination so that the lesions can be anticipated and that an organized treatment plan can be developed.8 9
The pathological sequelae of bowel obstruction progress rapidly and are poorly tolerated by most neonates.4 10 However, early diagnosis and treatment lead to better outcome.5 6 Similarly, surgery in neonates is still a challenging issue, especially in low-income countries.7 11 12 Neonates usually require surgical management by trained pediatric surgeons in centers equipped with specialized anesthetic and neonatal intensive care.5 13 This is usually not the case in many settings, and hence nearly 25% of the neonates with obstruction suffer complications, such as sepsis, surgical site infection, and an anastomotic leak in their early postoperative period.10 14
Each year, about 2.5 million children die within the first month of life worldwide, and in Uganda, neonatal mortality has remained as high as 34 per 1000 live births during the past decade, with very little attention given to surgical causes.15–17 Ullrich et al reported neonatal mortality of 36% among neonates with surgical conditions in Uganda, predominantly among cases of ARM (37%) and JIA (38%).16 A report by Cairo et al indicated a mortality rate of 43% among neonates with intestinal atresia.18 These figures are quite high compared to the findings in Europe, where a mortality is less than 15% among neonates with obstruction.3 9
With such glaring disparities in mortality, there is a huge need to understand the high rate and more specially to identify the predictors, which are not well elucidated in our setting. Therefore, our aims were to describe the etiological spectrum and early postoperative outcomes and to determine the predictors of mortality due to bowel obstruction among neonates. We believe the findings will inform decision-making that will reduce the morbidity and mortality due to bowel obstruction among neonates.
Methods
We conducted a prospective cohort study at the pediatric surgery unit of Mulago Hospital, a national referral hospital in Uganda, and a teaching hospital for Makerere University College of Health Sciences. The sample size of 76 was calculated using the Fleiss formula (1981). This was compared to a study that assessed the predictors of mortality among children with bowel obstruction in Mulago Hospital (Naluyimbazi19). The Fleiss formula is as follows:
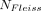 =
= 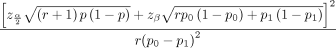
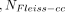 =
= 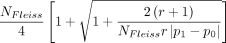 , P =
, P =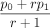
Where α=0.05, the probability of type I error (significance level) is the probability of rejecting the true null hypothesis; β=0.2, the probability of type II error (1−power of the test) is the probability of rejecting a true alternative hypothesis; p0=0.153 (15.3% of the children with bowel obstruction who had no perforation died according to the study by Naluyimbazi19); p1=0.667 (66.7% of the children with bowel obstruction who had a perforation died according to the study by Naluyimbazi19); r=0.1, the ratio of exposed to unexposed; NFleiss−cc=76 required sample size for the unexposed group using Fleiss formula with continuity correction; N2=0.1×76=8, the required sample size=8+76=84. We recruited 76 neonates (within 10% of the requirement) during a period of 4 months.
All participants had standard preoperative care including blood workup and plain abdominal X-ray. We ensured treatment, such as warm care, fluid deficit correction, antibiotic therapy, and other care. All participants underwent an operation as early as possible after optimization. Care such as fluid therapy, antibiotics, and pain management was instituted after the surgery. The participants were followed up while noting the outcome of interest. Survival during a 2-week postoperative period was taken as the end point for analysis. The differences in the proportions of the causes of obstruction were compared across various demographics using Fisher’s exact test at a p<0.05. We obtained the hazard ratios (HRs) and their 95% Confidence intervals (CIs) using Cox proportional hazards regression analysis, and we considered significant regressors as those which achieved a p<0.05 in the multivariate analysis.
Results
Baseline characteristics
A total of 76 neonates were recruited, with a male-to-female ratio of 2.2:1 and an age range of 1–26 days, a median of 3 [interquartile range (IQR): 2, 7]. Most birth weights (67.1%) ranged between 2.5 kg and 3.5 kg, a mean of 2.81 kg [standard deviation (SD)=0.6]. About 76.3% of the neonates were born full term. The majority (71.1%) had a history of fever, with temperatures ranging from 35.5°C to 39°C, a mean of 37.3°C (SD=0.8). Most neonates were referrals (96%), and mainly from multiparous mothers (71.1%). Stoma placement was the most common procedure performed, 45 (59.2%), and most operations were carried out by pediatric surgery fellows, 38 (50%) (table 1).
Baseline characteristics
Etiological spectrum
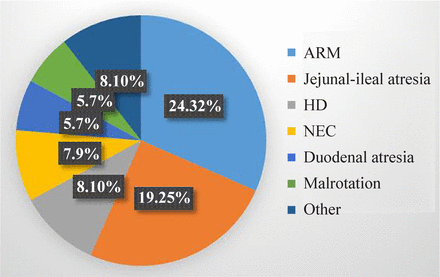
Various causes of obstruction were identified with ARM affecting the highest number, 24/76 (31.6%) followed by Jejunoileal atresia (JIA) at 19/76 (25.0%). The remainder are as shown in figure 1.
Distribution of the various causes of bowel obstruction. ARM, anorectal malformation; HD, Hirschsprung’s disease; NEC, necrotizing enterocolitis.
Fisher’s exact test found that patients’ age at presentation and gestation were significant different among groups with different causes of bowel obstruction with p values of <0.001 and 0.005, respectively (table 2).
Distribution of the causes of obstruction by demographics
A relatively high proportion with ARM (48.8%) and JIA (26.8%) was among the early presenters (within 3 days of life). In addition, many with HD and NEC presented after their third day of life (p<0.001). Most cases of ARM (39.7%) and HD (13.8%) were delivered at term, whereas many with JIA (44.4%), duodenal atresia (16.7%), NEC, and malrotation were pretermed (p=0.005). Male participants predominated among cases of ARM and HD, yet female participants predominated among JIA, NEC, duodenal atresia, and malrotation (though not significant).
Early postoperative outcomes
Nearly 55.3% experienced complications in the early postoperative period, and a higher proportion developed postoperative fever, 53.9% with 15.8% getting surgical site infection. The various outcomes were compared across the various causes of bowel obstruction using Fisher’s exact test at a p-value <0.005, where post-operative fever and anastomotic leaks were significant with p-values of 0.002 and <0.001, respectively (table 3).
Early postoperative outcomes
Many neonates with JIA (61.5%) and NEC (25.2%) experienced complications in the early postoperative period, unlike in other forms of bowel obstructions (though not statistically significant). Anastomotic leak was noticed commonly among cases of JIA (75%) and malrotation (25%), p<0.001, whereas postoperative fever was noticed more among cases of NEC (22.7%) and HD (22.7%), p=0.002. Many neonates with NEC and JIA had wound dehiscence too (though not significant).
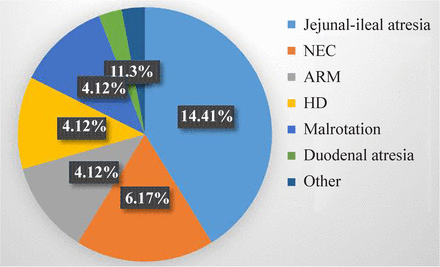
After the operation, time to discharge or death was recorded with a range of 1–12 days, a mean of 4.3 days (SD=2.4) and median of 4 days (IQR: 3, 5). Status at discharge showed 34 (44.7%) neonates had died; JIA had the highest mortality rate of 41.2% followed by NEC at 17% (figure 2).
Distribution of deaths by cause of obstruction. ARM, anorectal malformation; HD, Hirschsprung’s disease; NEC, necrotizing enterocolitis.
Predictors of mortality
Variables with p<0.2 in the univariate analysis were considered for multivariate analysis. These variables included age, history of fever, mother’s parity, gestational age, and birth weight and breastfeeding status. We determined the relationship between predictors and the outcome using Cox proportional hazard regression analysis, where age at presentation, fever at admission, mother’s parity, gestational age among others were significant with p-values <0.005 (table 4).
Multivariate analysis for predictors of mortality
Preterm neonates had more than 7 times higher risk of dying than termed neonates (aHR=7.56, 95% CI=2.50 to 22.86, p≤0.001). Neonates with fever at admission had more than 3 times higher risk of dying (aHR=3.53, 95% CI=1.29 to 9.62, p=0.014). Meanwhile, neonates from multiparous mothers had 69% more chances of survival than their counterparts (aHR=0.31, 95% CI=0.01 to 0.97, p=0.044); and neonates who were exclusively breast fed had 66% more chances of survival than those on mix feeds (aHR=0.34, 95% CI=0.12 to 0.96, p=0.043). Similarly, neonates above 3 days old had a higher survival rate (86%) following surgery compared with those below 3 days (aHR=0.14, 95% CI=0.05 to 0.43, p=0.001). Neonates operated on by pediatric surgeons had better chances of survival (85%) than those operated on by other cadres (aHR=0.15, 95% CI=0.04 to 0.53, p=0.003).
Discussion
Etiological spectrum
Bowel obstruction among neonates, including those in our series, is mainly due to congenital origin.1–3 9 ARM was the leading cause in our series, which agrees with reports from other series though not in others in which JIA was the most common cause.2–4 16 20 We also noticed that many with ARM reported within 3 days of life, the fact that most of them, especially those with no perianal fistula get early symptoms. This result concurs with other related reports too.7 10 In addition, most neonates with ARM were delivered at term, with a male-to-female ratio of 5:1, which agrees with many authors as well.5 13
JIA was second highest cause of bowel obstruction, although it predominated among cases of atresia, which was concordant with reports in other series with a male-to-female ratio of 1:1.7–9 JIA is believed to be a common finding among the premature which is about the same as ours, where about 44% were preterm.4 21 Similarly, presentation in atresia is usually early, within 7 days, and this was in agreement with our findings in which most cases of JIA presented within 3 days with exception of a few cases of duodenal atresia who presented after their third day, though would still be within 7 days.21–23 We think that the early onset of symptoms and rapid deterioration of the patient’s condition in atresia is the probable cause of early presentation. These findings, however, were not in agreement with the report by Cairo et al, wherein many neonates with intestinal atresia presented after day 7.18
HD, on the other hand, was a major cause of obstruction in other reports, but in our study the incidence was low.4 11 A study conducted by Saha et al showed a 35.3% incidence of HD, higher than that of atresia, whereas in other related studies the incidence was almost equal, with HD leading over atresia.3 10 11 In this series, all cases of HD were male; and most termed, a concordant finding with other literature, where HD was found to be more common among male babies.12 22 However, most cases of HD presented late, with a median age of 12 days, which is later than the median age of 6 days in similar series.3 8 Presentation in HD is usually delayed owing to variability in the onset of symptoms and lack of specificity. This may lead to increased morbidity, though the prognosis is good even in late presenters because decompression is often done repeatedly by doing enema at peripheral centers.
Malrotation was the fifth leading cause with a male-to-female ratio of 1.5:1, a fewer incidence than in other reports, though about the same in some.5 11 21 Most malrotation cases presented within the first 3 days of life, but this result does not agree with related series where neonates with malrotation were termed late presenters.13 14 On the other hand, neonates with NEC usually present late, as in our series, where many presented after the third day.7 14 As in JIA, NEC is common among premature, a finding that agrees with ours, with a male-to-female ratio of 1.5:1. In our series, many with NEC were on mixed feeds.11 24
Meconium ileus was one of the most common causes of obstruction as noted by Saha et al, whereas cases of meconium ileus were quite a few in ours.11 This could be due to the low incidence of cystic fibrosis in the region, which is usually the cause of meconium ileus. Other less common causes of bowel obstruction in our series included obstructed hernia and bowel stenosis as in other series.4 5 11 13 Overall, in our series ‘low’ obstruction was observed more often than the ‘high’ types, unlike in others.12 14 We do not have a clear reason for this and hence may require validation with subsequent studies.
Early postoperative outcomes
About 55% of the neonates in our series developed complications in the early postoperative period, which concurs with related series in sub-Saharan Africa, though does not agree with the report from high-income countries.5 11 14 21 25 Of these, nearly 69% died and only 31% were discharged alive. However, close to 15% of the neonates without complications died as well. This result was attributed to neonates which died in the immediate postoperative period, probably as a result of anesthesia-related complications. Others could be due to complications, such as prematurity, severe congenital anomalies, or inadequate optimization before surgery.
We noticed higher morbidity among cases of NEC and malrotation, as in other series where most of these cases were late presenters with the risk of poor prognosis as a result of repeated vomiting and electrolyte imbalances.19 26 In addition, most of these were referrals from peripheral health facilities, where services are not equipped to detect obstruction at an early stage leading to delayed presentation. Similarly, neonates with JIA also had higher morbidity, as most of these were neonates premature; thus, the risk of dying during the perioperative period was probably due to complications associated with prematurity. This concurs with reports from related series.15 26
At least 50% of neonates in our series developed persistent fever after 24 hours of surgery, attributed to sepsis; commonly among cases of NEC and HD, a finding quite high compare to other series.12 24 Neonates with NEC often present with sepsis following peritonitis; and if not optimized well, will have fever in the postoperative phase. Meanwhile those with HD, despite being late presenters with the risk of sepsis, do get HD-associated enterocolitis which may present with fever too. However, mild postoperative fever (<38°C) could be due to physiological changes, especially within 48 hours of surgery.
Nearly 16% of neonates in our study had surgical site infection, commonly among cases of JIA and HD, which was in line with findings from related studies.5 21 The explanation could be due to poor hygiene and improper wound care because most of these neonates were mainly born to first-time mothers. On the other hand, the few who developed anastomotic leaks were mostly among cases of JIA and malrotation because most of these underwent resection and anastomoses.
Electrolyte imbalances also have been reported as a major outcome.5 13 In our series, many presumably died due to electrolyte derangement, though we think the actual figure could be less than what was reported because most of the time we practice rigorous preoperative correction of the deficit. However, many had features of sepsis, and yet the majority of neonatal sepsis has electrolyte abnormalities; hence, some could have had electrolyte imbalances and died unnoticed.
The mortality due to bowel obstruction among neonates ranges between 21% and 45% in low-income and middle-income countries, unlike <15% in Europe.25 26 In our series, the mortality was about 45%, which is within the above range. However, a similar report by Hanif et al, observed postoperative mortality of 15.4%, just like a finding from a study conducted by Islam et al in which mortality of 20.8% was reported.14 22 In the same context, Ullrich et al also noted a postoperative mortality rate of 37% and 38% among cases of ARM and JIA, respectively.16 However, in our series, we noticed higher mortality among cases of JIA and NEC. These were the same categories who developed fever and anastomotic leak after surgery, in addition to some of them being premature.
Predictors of mortality
Neonates with fever at admission, attributed to sepsis, had less chance of survival. This result agrees with that of other authors where sepsis was a major predictor of mortality.5 10 11 13 24 Premature babies also had a poor prognosis, as in other series, because these babies are prone to hypothermia, hypoglycemia, and sepsis.14 26 27 Similarly, neonates who presented within the first 3 days of life were more at risk of dying because being early presenters may indicate a very severe symptoms that making them prone to complications in the early postoperative phase. However, because in most series the mortality rates were higher in late presenters, this may require further validation with subsequent studies.4 14 21 22 25 Most neonates from primipara mothers in our series had lower survival rate. As hinted at by Kidus et al, most first-time mothers do not know how to care for the newborn, especially during the perioperative period.28 In the same way, we noted that neonates on mixed feeds had higher mortality too because they are usually prone to NEC, especially the extremely low birth weight, as was noted by Colaizy et al.29 Furthermore, the type of surgery performed affects the outcome, where stoma placement is associated with a reduction in mortality, especially in intestinal atresia.4 21 This was not the case in our study. We had many with a stoma but still had unacceptably high mortality, though these were primarily for the cases of ARMs as the initial treatment care. The anastomotic leak, unlike in our series, has been noted as a major predictor of mortality. A baby who develops a leak carries a risk of sepsis as well as electrolyte derangement.10 19 Similarly, the anastomotic leak has also been linked to the cadre of healthcare providers who do these operations.4 10 In line with that, Rhee et al noted that most neonates operated on by pediatric surgeons have less risk of anastomotic leak, with a better outcome, which is a similar finding in our series.30
Obstruction in association with multiple congenital anomalies, though not present in our study, has been reported in other series as a major predictor of mortality.10 11 13 14 21 Neonates with congenital heart defects pose challenges to the anesthesia team because some of these neonates may require prolonged respiratory support. Causes of obstruction and the duration of surgery have also been noted by other authors as predictors of mortality.5 12 We did not notice these, comparable to report of other authors.15 19 24
In conclusion, anorectal malformation is still the leading cause of bowel obstruction yet morbidity and mortality among these neonates is unacceptably high with the major predictors of mortality being age at presentation, prematurity, fever at admission, mothers’ parity, and breastfeeding status.
Limitations
Selection bias could have been introduced into the study by non-probability sampling. However, this bias was kept at a minimum because there was no loss to follow-up. The type of obstruction, as well as the surgery performed, could have affected the outcome in these neonates, though was catered for at the analysis level. The findings in this study may not be representative of all the neonates with bowel obstruction in the region due to limited sample size and hence may require a multicenter study for validation.
Recommendations
We recommend that premature neonates and neonates with fever at admission need to be optimized properly prior to surgery, and preferably they need to be operated on by pediatric surgeons. Further studies should be conducted to confirm the validity of the major predictors of mortality that we identified. This will help in reducing any bias in our conclusions due to limited sample size of our study.
Data availability statement
Data are available upon reasonable request. The data used to support the findings of this study are available from the corresponding author upon request.
Ethics statements
Patient consent for publication
Ethics approval
This study involves human participants and was approved by Makerere University College of Health Sciences, School of Medicine Research, and ethics committee (REC REF 2020-018). Participants gave informed consent to participate in the study before taking part.
Acknowledgments
We thank the staff of the department of surgery, Makerere University College of Health Sciences, and all the health workers of Mulago Hospital who participated in one way or another in this study. In particular, we appreciate the lead research assistant, Sr Adong Stella, for her tireless effort.
References
Footnotes
Contributors PO did conceptulisation,investigation,writing original draft and he is the gurantor to this manucsript. EAE did Supervision and formal analysis. RM and NK contributed towards data curation and validation. DK did methodology,writing-review, editing and was the corresponding author.
Funding The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Competing interests None declared.
Provenance and peer review Not commissioned; externally peer reviewed.